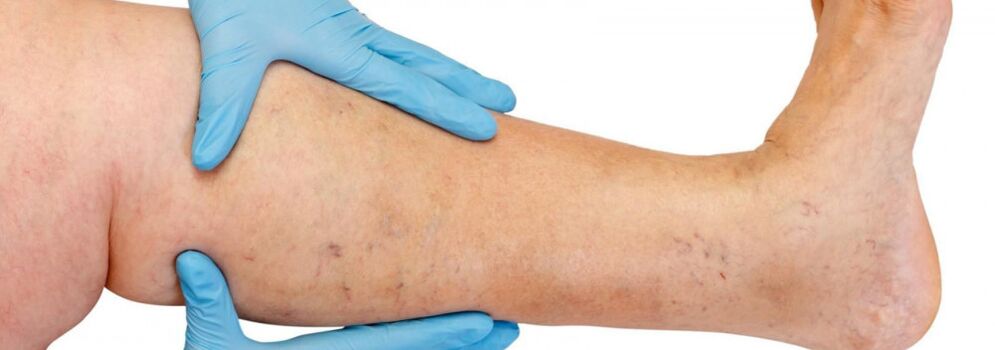
The anatomical structure of the venous system of the lower extremities is characterized by great variability.Knowledge of the individual characteristics of the structure of the venous system plays a big role in assessing instrumental examination data and in choosing the correct treatment method.
The veins of the lower extremities are divided into superficial and deep.The superficial venous system of the lower extremities begins from the venous plexuses of the toes, forming the venous network of the dorsum of the foot and the cutaneous dorsal arch of the foot.From it originate the medial and lateral marginal veins, which pass into the greater and lesser saphenous veins, respectively.The great saphenous vein is the longest vein in the body, contains from 5 to 10 pairs of valves, and its normal diameter is 3-5 mm.It originates in the lower third of the leg in front of the medial epicondyle and rises in the subcutaneous tissue of the leg and thigh.In the groin area, the great saphenous vein drains into the femoral vein.Sometimes the great saphenous vein on the thigh and leg can be represented by two or even three trunks.The small saphenous vein begins in the lower third of the leg along its lateral surface.In 25% of cases, it flows into the popliteal vein in the area of the popliteal fossa.In other cases, the small saphenous vein can rise above the popliteal fossa and flow into the femoral, large saphenous vein, or into the deep vein of the thigh.
The deep veins of the dorsum of the foot begin with the dorsal metatarsal veins of the foot, which flow into the dorsal venous arch of the foot, from where blood flows into the anterior tibial veins.At the level of the upper third of the leg, the anterior and posterior tibial veins merge to form the popliteal vein, which is located lateral and somewhat posterior to the artery of the same name.In the area of the popliteal fossa, the small saphenous vein and the veins of the knee joint flow into the popliteal vein.The deep vein of the thigh usually flows into the femoral vein 6-8 cm below the inguinal fold.Above the inguinal ligament, this vessel receives the epigastric vein, the deep vein surrounding the ilium, and passes into the external iliac vein, which merges with the internal iliac vein at the sacroiliac joint.The paired common iliac vein begins after the confluence of the external and internal iliac veins.The right and left common iliac veins merge to form the inferior vena cava.It is a large vessel without valves, 19-20 cm long and 0.2-0.4 cm in diameter. The inferior vena cava has parietal and visceral branches, through which blood flows from the lower extremities, lower torso, abdominal organs, and small pelvis.
Perforating (communicating) veins connect the deep veins with the superficial ones.Most of them have valves located suprafascially and thanks to which blood moves from the superficial veins to the deep ones.There are direct and indirect perforating veins.Direct ones directly connect the deep and superficial venous networks, indirect ones connect indirectly, that is, they first flow into the muscular vein, which then flows into the deep vein.
The vast majority of perforating veins arise from tributaries rather than from the trunk of the great saphenous vein.In 90% of patients, there is incompetence of the perforating veins of the medial surface of the lower third of the leg.On the lower leg, incompetence of the perforating veins of Cockett, which connects the posterior branch of the great saphenous vein (vein of Leonardo) with the deep veins, is most often observed.In the middle and lower thirds of the thigh there are usually 2-4 most permanent perforating veins (Dodd, Gunter), directly connecting the trunk of the great saphenous vein with the femoral vein.With varicose transformation of the small saphenous vein, incompetent communicating veins of the middle, lower third of the leg and in the area of the lateral malleolus are most often observed.
Clinical course of the disease
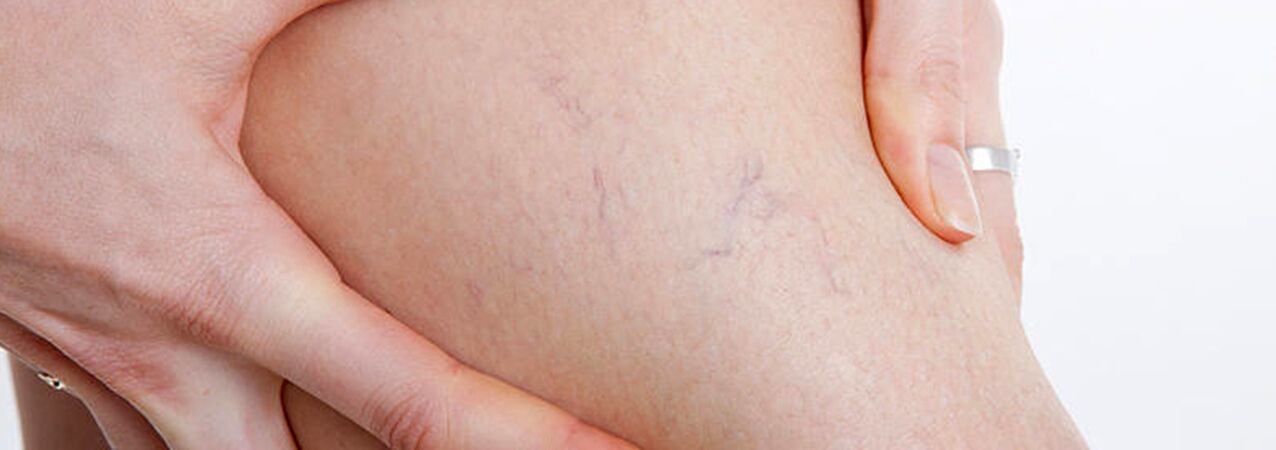
Mostly, varicose veins occur in the system of the great saphenous vein, less often in the system of the small saphenous vein, and begin with the tributaries of the vein trunk on the legs.The natural course of the disease at the initial stage is quite favorable; for the first 10 years or more, apart from a cosmetic defect, patients may not be bothered by anything.Subsequently, if timely treatment is not carried out, complaints of a feeling of heaviness, fatigue in the legs and their swelling after physical activity (long walking, standing) or in the afternoon, especially in the hot season, begin to appear.Most patients complain of pain in the legs, but upon detailed questioning it is possible to reveal that this is precisely a feeling of fullness, heaviness, and fullness in the legs.With even a short rest and elevated position of the limb, the severity of sensations decreases.It is these symptoms that characterize venous insufficiency at this stage of the disease.If we are talking about pain, it is necessary to exclude other causes (arterial insufficiency of the lower extremities, acute venous thrombosis, joint pain, etc.).Subsequent progression of the disease, in addition to an increase in the number and size of dilated veins, leads to the occurrence of trophic disorders, often due to the addition of incompetent perforating veins and the occurrence of valvular insufficiency of the deep veins.
In case of insufficiency of perforating veins, trophic disorders are limited to any of the surfaces of the leg (lateral, medial, posterior).Trophic disorders at the initial stage are manifested by local hyperpigmentation of the skin, then thickening (induration) of subcutaneous fatty tissue occurs until the development of cellulite.This process ends with the formation of an ulcerative-necrotic defect, which can reach a diameter of 10 cm or more, and extend deep into the fascia.The typical place of occurrence of venous trophic ulcers is the area of the medial malleolus, but the localization of ulcers on the lower leg can be different and multiple.At the stage of trophic disorders, severe itching and burning in the affected area occur;Some patients develop microbial eczema.Pain in the area of the ulcer may not be expressed, although in some cases it is intense.At this stage of the disease, heaviness and swelling in the leg become constant.
Diagnosis of varicose veins
It is especially difficult to diagnose the preclinical stage of varicose veins, since such a patient may not have varicose veins on the legs.
In such patients, the diagnosis of varicose veins of the legs is mistakenly rejected, although there are symptoms of varicose veins, indications that the patient has relatives suffering from this disease (hereditary predisposition), and ultrasound data on initial pathological changes in the venous system.
All this can lead to missed deadlines for the optimal start of treatment, the formation of irreversible changes in the venous wall and the development of very serious and dangerous complications of varicose veins.Only when the disease is recognized at an early preclinical stage does it become possible to prevent pathological changes in the venous system of the legs through minimal therapeutic effects on varicose veins.
Avoiding various kinds of diagnostic errors and making a correct diagnosis is possible only after a thorough examination of the patient by an experienced specialist, correct interpretation of all his complaints, a detailed analysis of the disease history and the maximum possible information about the state of the venous system of the legs obtained using the most modern equipment (instrumental diagnostic methods).
Duplex scanning is sometimes performed to determine the exact location of perforating veins, identifying venovenous reflux in a color code.In case of valve insufficiency, their valves stop closing completely during the Valsava maneuver or compression tests.Valve insufficiency leads to the appearance of venovenous reflux, high, through the incompetent saphenofemoral junction, and low, through the incompetent perforating veins of the leg.Using this method, it is possible to record the reverse flow of blood through the prolapsed leaflets of an incompetent valve.That is why diagnosis is multi-stage or multi-level.In a normal situation, the diagnosis is made after ultrasound diagnostics and examination by a phlebologist.However, in particularly difficult cases, the examination must be performed in stages.
- First, a thorough examination and questioning is carried out by a phlebologist surgeon;
- if necessary, the patient is sent for additional instrumental research methods (duplex angioscanning, phleboscintigraphy, lymphoscintigraphy);
- patients with concomitant diseases (osteochondrosis, varicose eczema, lymphovenous insufficiency) are offered consultation with leading specialist consultants on these diseases) or additional research methods;
- all patients requiring surgery are first consulted by the operating surgeon and, if necessary, by an anesthesiologist.
Treatment
Conservative treatment is indicated mainly for patients who have contraindications to surgical treatment: due to their general condition, with slight dilation of the veins causing only cosmetic inconvenience, or if surgical intervention is refused.Conservative treatment is aimed at preventing further development of the disease.In these cases, patients should be advised to bandage the affected surface with an elastic bandage or wear elastic stockings, periodically place their legs in a horizontal position, and perform special exercises for the foot and lower leg (flexion and extension in the ankle and knee joints) to activate the muscular-venous pump.Elastic compression accelerates and enhances blood flow in the deep veins of the thigh, reduces the amount of blood in the saphenous veins, prevents the formation of edema, improves microcirculation, and helps normalize metabolic processes in tissues.Bandaging should begin in the morning, before getting out of bed.The bandage is applied with slight tension from the toes to the thigh, with the obligatory grip of the heel and ankle joint.Each subsequent round of the bandage should overlap the previous one by half.It is recommended to use certified medical knitwear with individual selection of the degree of compression (from 1 to 4).Patients should wear comfortable shoes with hard soles and low heels, avoid prolonged standing, heavy physical labor, and work in hot and humid areas.If, due to the nature of the work activity, the patient has to sit for a long time, then the legs should be placed in an elevated position by placing a special stand of the required height under the feet.It is advisable to walk a little every 1-1.5 hours or stand on your toes 10-15 times.The resulting contractions of the calf muscles improve blood circulation and increase venous outflow.During sleep, your legs need to be placed in an elevated position.
Patients are advised to limit their intake of water and salt, normalize body weight, and periodically take diuretics and drugs that improve venous tone.According to indications, medications are prescribed that improve microcirculation in tissues.For treatment, it is recommended to use non-steroidal anti-inflammatory drugs.
Physical therapy plays a significant role in the prevention of varicose veins.For uncomplicated forms, water procedures are useful, especially swimming, warm (not higher than 35°) foot baths with a 5-10% solution of table salt.
Compression sclerotherapy
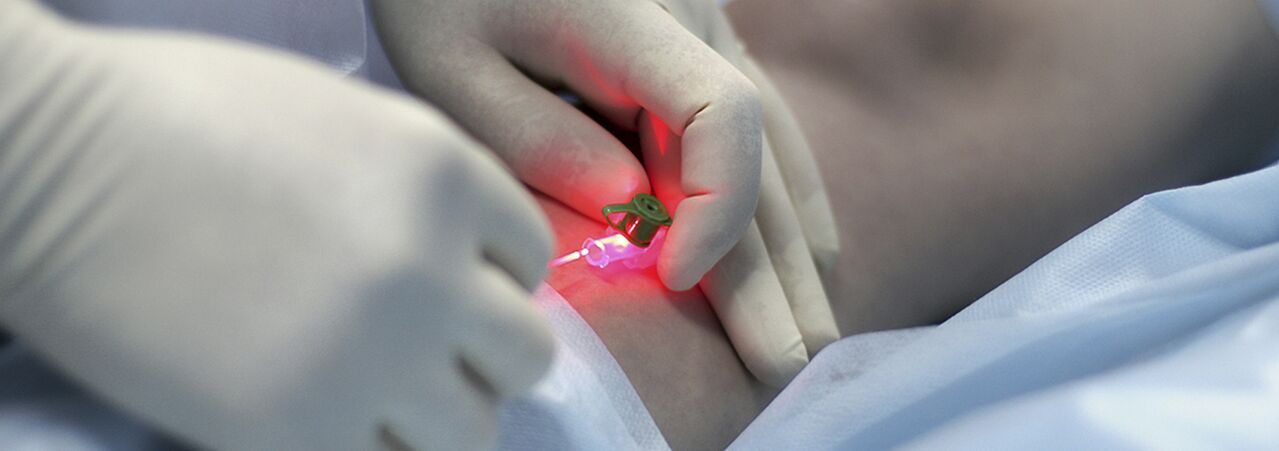
Indications for injection therapy (sclerotherapy) for varicose veins are still being debated.The method consists of introducing a sclerosing agent into the dilated vein, its further compression, desolation and sclerosis.Modern drugs used for these purposes are quite safe, i.e.do not cause necrosis of the skin or subcutaneous tissue when administered extravasally.Some specialists use sclerotherapy for almost all forms of varicose veins, while others reject the method completely.Most likely, the truth lies somewhere in the middle, and it makes sense for young women with the initial stages of the disease to use the injection method of treatment.The only thing is that they must be warned about the possibility of relapse (higher than with surgical intervention), the need to constantly wear a fixing compression bandage for a long time (up to 3-6 weeks), and the likelihood that several sessions may be required for complete sclerosis of the veins.
The group of patients with varicose veins should include patients with telangiectasias (“spider veins”) and mesh dilatation of small saphenous veins, since the causes of the development of these diseases are identical.In this case, along with sclerotherapy, you can alsopercutaneous laser coagulation, but only after excluding damage to the deep and perforating veins.
Percutaneous laser coagulation (PLC)
This is a method based on the principle of selective photocoagulation (photothermolysis), based on the different absorption of laser energy by various substances in the body.A special feature of the method is the non-contact nature of this technology.The focusing head concentrates energy into a blood vessel in the skin.Hemoglobin in the vessel selectively absorbs laser beams of a certain wavelength.Under the action of a laser, destruction of the endothelium occurs in the lumen of the vessel, which leads to gluing of the vessel walls.
The effectiveness of PLK directly depends on the depth of penetration of laser radiation: the deeper the vessel is, the longer the wavelength should be, thus PLK has rather limited indications.For vessels with a diameter exceeding 1.0-1.5 mm, microsclerotherapy is most effective.Considering the extensive and branched distribution of spider veins on the legs and the variable diameter of the vessels, a combined treatment method is currently actively used: at the first stage, sclerotherapy of veins with a diameter of more than 0.5 mm is performed, then a laser is used to remove the remaining “stars” of a smaller diameter.
The procedure is practically painless and safe (skin cooling and anesthetics are not used), since the light of the device belongs to the visible part of the spectrum, and the light wavelength is designed so that the water in the tissues does not boil and the patient does not receive burns.For patients with high pain sensitivity, preliminary application of a cream with a local anesthetic effect is recommended.Erythema and swelling subside within 1-2 days.After the course, for about two weeks, some patients may experience darkening or lightening of the treated area of skin, which then disappears.In people with fair skin, the changes are almost unnoticeable, but in patients with dark skin or a strong tan, the risk of such temporary pigmentation is quite high.
The number of procedures depends on the complexity of the case - the blood vessels are at different depths, the lesions can be minor or occupy a fairly large surface of the skin, but usually no more than four laser therapy sessions are needed (5-10 minutes each).The maximum result in such a short time is achieved due to the unique “square” shape of the light pulse of the device; it increases its effectiveness compared to other devices, also reducing the possibility of side effects after the procedure.
Surgical treatment
Surgery is the only radical treatment method for patients with varicose veins of the lower extremity.The purpose of the operation is to eliminate pathogenetic mechanisms (veno-venous reflux).This is achieved by removing the main trunks of the great and small saphenous vein and ligating the incompetent communicating veins.
Surgical treatment of varicose veins has a hundred-year history.Previously, and many surgeons still do, large incisions along the varicose veins and general or spinal anesthesia were used.Traces after such a “mini-phlebectomy” remain a lifelong reminder of the surgery.The first operations on veins (according to Schade, according to Madelung) were so traumatic that the harm from them exceeded the harm from varicose veins.
In 1908, the American surgeon Babcock came up with a method of subcutaneous vein pulling using a rigid metal probe with an olive.In an improved form, this method of surgery for removing varicose veins is still used in many public hospitals.Varicose veins are removed using separate incisions, as suggested by surgeon Narat.Thus, classical phlebectomy is called the Babcock-Narat method.Phlebectomy according to Babcock-Narat has disadvantages - large scars after surgery and impaired skin sensitivity.Working capacity is reduced for 2-4 weeks, which makes it difficult for patients to agree to surgical treatment of varicose veins.
Phlebologists have developed a unique technology for treating varicose veins in one day.Complex cases are operated on usingcombined technology.The main large varicose trunks are removed by inversion stripping, which involves minimal intervention through mini-incisions (from 2 to 7 mm) of the skin, which leave virtually no scars.The use of a minimally invasive technique involves minimal tissue trauma.The result of this operation is the elimination of varicose veins with an excellent aesthetic result.Combined surgical treatment is performed under total intravenous or spinal anesthesia, with a maximum hospitalization period of up to 1 day.
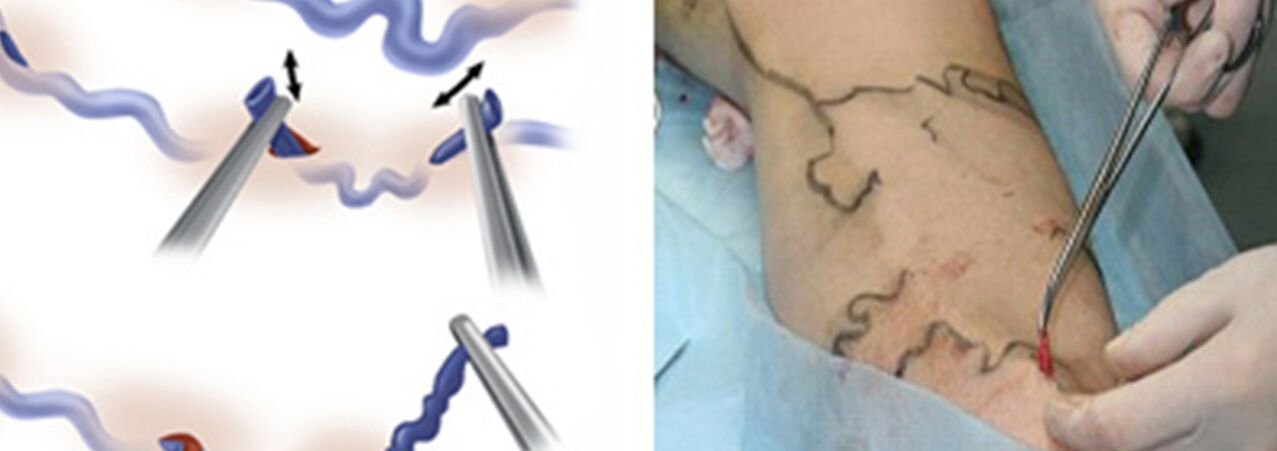
Surgical treatment includes:
- Crossectomy - crossing the place where the trunk of the great saphenous vein flows into the deep venous system;
- Stripping is the removal of a varicose vein fragment.Only the varicose vein is removed, and not the whole one (as in the classic version).
Actuallyminiphlebectomyreplaced the Narat technique for removing varicose tributaries of the main veins.Previously, skin incisions from 1-2 to 5-6 cm were made along the course of varixes, through which the veins were isolated and removed.The desire to improve the cosmetic result of the intervention and to be able to remove veins not through traditional incisions, but through mini-incisions (punctures), forced doctors to develop tools that allow them to do almost the same thing through a minimal skin defect.This is how sets of phlebectomy “hooks” of various sizes and configurations and special spatulas appeared.And instead of a regular scalpel, scalpels with a very narrow blade or needles of a fairly large diameter began to be used to pierce the skin (for example, a needle used to take venous blood for analysis with a diameter of 18G).Ideally, the mark of a puncture with such a needle is practically invisible after some time.
Some forms of varicose veins are treated on an outpatient basis under local anesthesia.Minimal trauma during miniphlebectomy, as well as a low risk of intervention, allows this operation to be performed in a day hospital.After minimal observation in the clinic after surgery, the patient can be sent home on their own.In the postoperative period, an active lifestyle is maintained, active walking is encouraged.Temporary incapacity for work usually lasts no more than 7 days, then it is possible to begin work.
When is microphlebectomy used?
- When the diameter of varicose trunks of the large or small saphenous vein is more than 10 mm;
- After suffering thrombophlebitis of the main subcutaneous trunks;
- After recanalization of the trunks after other types of treatment (EVLT, sclerotherapy);
- Removal of very large individual varicose veins.
It can be an independent operation or be a component of a combined treatment of varicose veins, combined with laser treatment of veins and sclerotherapy.The tactics of use are determined individually, always taking into account the results of ultrasound duplex scanning of the patient’s venous system.Microphlebetomy is used to remove veins of various locations that have changed for various reasons, including on the face.Professor Varadi from Frankfurt developed his convenient instruments and formulated the basic postulates of modern microphlebectomy.The Varadi phlebectomy method provides excellent cosmetic results without pain or hospitalization.This is very painstaking, almost jewelry work.
After vein surgery
The postoperative period after the usual “classical” phlebectomy is quite painful.Sometimes large hematomas are a concern, and swelling occurs.Wound healing depends on the surgical technique of the phlebologist; sometimes there is a leakage of lymph and long-term formation of noticeable scars; often after a major phlebectomy there remains a loss of sensitivity in the heel area.
In contrast, after a miniphlebectomy, wounds do not require suturing, since these are only punctures, there is no pain, and no damage to the cutaneous nerves has been observed in practice.However, such results of phlebectomy are achieved only by very experienced phlebologists.























